Opioids provide powerful relief from pain, but their many serious side effects include a paradoxical increase in pain, a phenomenon referred to as opioid-induced hyperalgesia (OIH), in patients and animals. Although OIH generally occurs with use of opioids over time, it has been reported following acute use of opioids after surgery. New work now shows that hyperalgesia can develop after even a single dose of morphine in rats.
Researchers led by Jon Levine at the University of California, San Francisco, US, demonstrate that low- and high-dose opioids activate distinct signaling pathways in nociceptive sensory neurons, leading to pain hypersensitivity. Rats displayed OIH after a single low dose of morphine, and both low- and high-dose morphine produced hyperalgesic priming, a phenomenon characterized by prolonged sensitivity to a subsequent inflammatory insult and thought to contribute to pain chronification. The team found that OIH and priming induced by low-dose morphine depended on signaling through the immune receptor toll-like receptor 4 (TLR4) in sensory neurons.
“I’m excited by the work,” said Mark Hutchinson, University of Adelaide, Australia, who studies the role of immune signaling in chronic pain but was not involved in the current study. “Clearly they’ve done some beautiful pharmacology here.” And, according to Hutchinson, the research represents a shift in thinking about opioid signaling. “Finally we are having a real debate around the question of whether we can assume that opioid agonists act only at opioid receptors. I take a lot of encouragement from the fact that there is discussion beyond just opioid receptors.”
The paper was published August 14, 2019, in the Journal of Neuroscience.
Priming: a model of chronic pain
Levine’s team had long aimed to understand the mechanisms underlying pain chronification, but they realized that a definition of pain based on symptom duration was not very helpful when trying to understand those mechanisms.
“Chronic pain is customarily defined as pain that lasts longer than some period of time, be it three months, six months, a year. As researchers trying to understand its mechanisms, that didn't make any sense to us. So we wanted to make a model to allow the study of the transition from acute to chronic pain from a mechanistic point of view—where time itself was not a central tenet to the diagnosis of chronic pain.”
With that in mind, Levine and colleagues previously developed a model they refer to as “hyperalgesic priming” (Aley et al., 2000). “We injected animals with PGE2,” referring to the pro-inflammatory signal prostaglandin E2 (PGE2), and “they had hyperalgesia that lasted less than an hour,” Levine explained. “But when we took an animal that had peripheral neuropathy, prior inflammation, or stress-induced pain, PGE2 caused hyperalgesia and tenderness that persisted for orders of magnitude longer.”
Because presurgical use of opioids has been implicated as a risk factor for the development of postoperative pain, the researchers thought that opioids might also induce priming. The new work builds on an earlier paper in which the group tested the effects of a single dose of morphine in naïve rats, from very low to high doses (Ferrari et al., 2019). Remarkably, a single injection of low-dose morphine (0.03 mg/kg) produced acute hyperalgesia in the animals.
“We didn’t have any idea that would happen,” said first author of the new work, Dioneia Araldi, also of UCSF. “It was very surprising, as there was no precedent in the literature,” she continued. “Researchers typically study the effects of chronic administration of high doses of opioids.”
“There is a novelty to it,” Hutchinson said of the hyperalgesia resulting from a low-dose opioid, and yet, he added, “nothing surprises me anymore” when it comes to opioid effects.
Araldi said their earlier work also showed “that high-dose morphine induced hyperalgesic priming and neuroplasticity in neurons.” Analgesia and priming by high-dose morphine depended on its action at mu opioid receptors (MORs). In contrast, Araldi said, “low-dose morphine induced hyperalgesia and priming, but they were not mediated by the mu opioid receptor.”
Another player
In the new work, Araldi and colleagues tested whether low-dose opioids might produce hyperalgesia through TLR4, an immune receptor that mediates multiple side effects of opioids, particularly in the central nervous system (e.g., see Wang et al., 2012).
The researchers treated naïve male rats intrathecally with an oligodeoxynucleotide (ODN) antisense (AS) to TLR4, reducing its expression by 22 percent in sensory ganglia. After three days of treatment with AS-ODN to TLR4 or a control ODN, rats were injected with low-dose morphine (LDM; 0.03 mg/kg) and then tested for mechanical nociceptive thresholds over the next hour. Control rats developed hyperalgesia, but those receiving AS-ODN to TLR4 did not. A day later, rats were injected with PGE2, which produced hyperalgesia 30 minutes later in all rats. Only control rats, however, still displayed hyperalgesia four hours after the injection. The results indicated that TLR4 mediated both OIH and priming induced by LDM.
Araldi then performed the same experiments using high-dose morphine (HDM; 3 mg/kg), which showed that neither analgesia nor priming by HDM depended on TLR4.
Hutchinson said that finding vexed him, because his previous work has shown that opioid agonists seem to act at TLR4 with low affinity—or at high doses—whereas opioid agonist effects at MOR are high affinity (e.g., see Grace et al., 2014). “The main thing that I’m questioning from this current work is the discrepancy in the potency of the effects of morphine at TLR4, because that does not agree with our work. My take on this is, ‘I’m fascinated by it and I want to learn more,’ rather than, ‘I dismiss it and don’t understand it.’”
Hutchinson said it is important to consider the microenvironment of TLR4, the presence of co-localized and chaperone proteins, and ionic conditions. He has looked in the central nervous system, but “when you move to the periphery, it is way, way different. So does TLR4 function depend upon the microenvironment that TLR4 finds itself in? Maybe that’s where we’re seeing these differences between the central and peripheral nervous systems.”
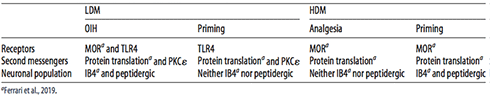

Opioids evoke multiple priming phenomena
In the current study, the authors also tested whether priming by LDM depended on protein kinase C epsilon (PKCε), which is required in some types of priming. Knockdown of PKCε prevented hyperalgesia and reduced the effects of priming by LDM, indicating that both processes required PKCε. Analgesia and priming by HDM, in contrast, were not affected by knockdown of PKCε.
To determine which neurons mediated the hyperalgesic effects of LDM, the researchers next injected rats intrathecally with the neurotoxin saporin to ablate specific nociceptor populations. Rats received IB4-saporin to destroy IB4-positive, non-peptidergic sensory neurons; SSP-saporin to kill peptidergic neurons; or a combination of both.
Two weeks later, rats that received either or both toxins did not display hyperalgesia in response to LDM as control rats did, indicating the phenomenon depends on sensory neurons including peptidergic and IB4-positive cells. Hyperalgesic priming by LDM, however, was not attenuated, suggesting that both classes of nociceptors were dispensable for priming. Levine suggested that a different class of sensory neurons may be primarily responsible for the action of LDM.
Analgesia produced by HDM was unaffected by sensory neuron ablation, as expected, because opioids work at MORs in the central nervous system to quell pain. The prolonged hyperalgesia induced by PGE2 injection following priming by HDM was attenuated in rats that received SSP-saporin and slightly reduced in those that received IB4-saporin. That suggested that in HDM-primed animals, prolonged PGE2 hyperalgesia was mediated by peptidergic and non-peptidergic sensory neurons.
Together, the experiments point to distinct mechanisms underlying the phenomena evoked by LDM and HDM that lead to pain hypersensitivity via drug actions at pain sensory neurons.
“I’m really excited that another group, using a fundamentally different model, has settled upon the concept that opioid agonists do not always act at opioid receptors,” Hutchison said. “Then the question is, What’s the clinical relevance? I don't know that, and we haven’t yet seen how this work fits together with relevance to repeated dosing with oral opioid agonists” in people. The work “paints more of that complexity to the story.”
Stephani Sutherland, PhD, is a neuroscientist and freelance journalist in Southern California. Follow her on Twitter @SutherlandPhD
Image credit: pixelrobot/123RF Stock Photo.